Practical Ways to Revitalize a Dull Smile Without Damaging Enamel
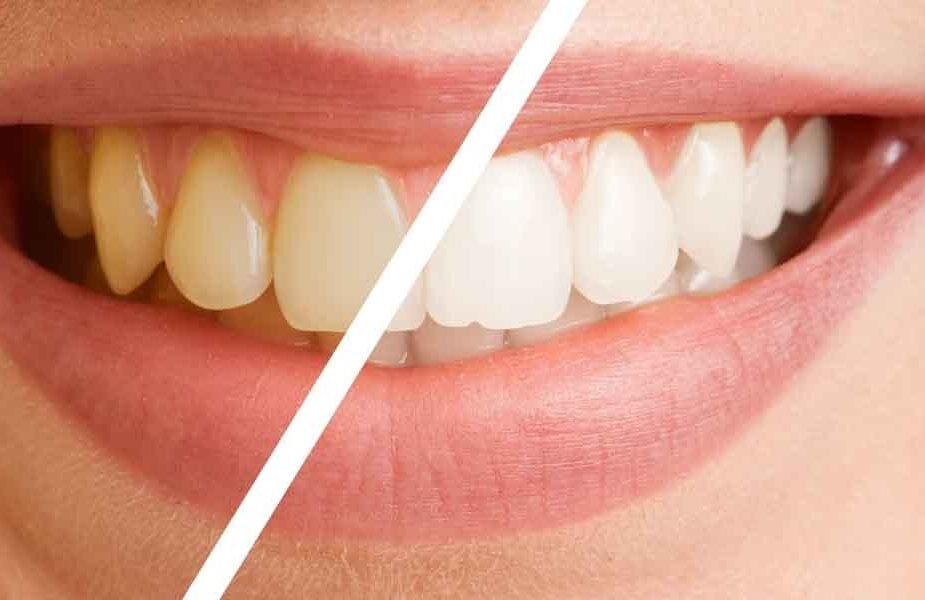
A lackluster or yellowed smile is seldom a strictly aesthetic concern – it can indicate more serious health problems that require attention before pursuing any whitening treatment. But many people grab a whitening strip or charcoal toothpaste without considering the source of the discoloration, and that’s where it all goes south. The type of stain determines the treatment.
Surface stains vs. deeper discoloration
External stains are on the enamel and caused by coffee, wine, and tobacco. They can often be removed by cleaning and whitening toothpaste. Internal stains are in the dentin, which is the layer under the enamel. Standard cleaning techniques won’t affect these deeper stains.
These two different kinds need different approaches. Trying to scrub out a stain in the dentin with a harsh whitening toothpaste would just wear out the enamel, which is the last thing you want. Before attempting any whitening treatments, you should have a deep-cleaning session with a dental hygienist to remove any plaque or tartar that could block the whitening gel from contacting your teeth evenly.
What a professional check-up actually changes
A dental assessment before whitening isn’t just a formality. Cavities and gum disease can both be made significantly worse by bleaching agents. Hydrogen peroxide and carbamide peroxide – the active compounds in whitening gels – penetrate through enamel. If there’s an existing cavity, the gel reaches the pulp, which causes sharp pain and can accelerate tissue damage. Inflamed gum tissue exposed to high-concentration bleaching agents is a direct route to gingival irritation and prolonged sensitivity.
Over-the-counter strips have a ceiling on what they can safely contain. For deep-set or intrinsic discoloration, seeking professional teeth whitening at a dentist is the only way to ensure the concentration of active ingredients is both strong enough to be effective and controlled enough to avoid enamel damage. Custom-fit trays, made from a precise mold of your teeth, also keep the gel off the gum tissue – something a one-size strip can’t guarantee.
High-street whitening parlours operate outside dental regulation in most jurisdictions. The staff aren’t trained to identify contraindications, and the products they use often contain concentrations that dental professionals are specifically trained to manage safely.
The real problem with DIY trends
People often share tips about using activated charcoal toothpastes or rinsing with lemon juice to whiten your teeth, but both suggestions are best avoided.
First, any dentist will tell you to steer clear of charcoal products. It’s not just a fad, but it’s actually confirmed by evidence. They’re incredibly abrasive, and their RDA value is quite high. The RDA value is a measure of how abrasive any substance is against the enamel. Products containing charcoal exist well over the approved safety threshold. If you use these products regularly, you’re effectively scrubbing the enamel away. You may notice some brightening in the short-term, but the dentin underneath (which incidentally is yellow) becomes more visible with continued use you’re not going to notice it “whitening” over time.
Likewise, lemon juice achieves the same ends through another route. Citric acid makes the mouth more acidic, softening the enamel by dropping the pH. This makes it easier to remove through both mechanical and enzymatic degradation. Purposely and repeatedly exposing your teeth to an acid isn’t the most tooth-friendly of ploys, no matter how many times you’ve read “it worked for me!” online.
Post-treatment care that most people skip
The 48 hours following a whitening session are the time when the teeth are, by far, most vulnerable to restaining. The treatment effectively – and temporarily – opens the pores in the enamel surface, so pigments from dark foods and drinks can more easily make their way inside. Sticking to a “White Diet” for two days following the session – with foods like chicken, rice, white fish, and dairy, while giving coffee, red wine, and tomato-based sauces a wide berth – gives the enamel a chance to reseal properly and protect the result.
Remineralization is the other somewhat under-discussed piece. Indeed, many whitening treatments can lead to a temporary form of dentin hypersensitivity, and by far the most effective way of managing that is with post-treatment remineralizing agents. Fluoride compounds and, particularly, calcium phosphates can help restore the mineral content of the enamel (kind of like fertilizing a lawn), which has the side effect of reducing that sensitivity, but also of strengthening the enamel toward future staining (acid erodes enamel easily) and acid exposure. Most good professional whitening protocols will provide you with a finishing application of a remineralizing gel, but it’s worth asking particularly if it’s a DIY kit.
Prioritizing the enamel you have
The intention of any whitening procedure must be a more luminous smile that does not harm your teeth in the long run. Unfortunately, enamel deterioration, ongoing pain, and gum issues are not unlikely results of inappropriate whitening. The good news is that the right choice of treatment, a preliminary examination, and proper post-whitening care can turn the process into a safe, suitable cosmetic treatment with long-lasting results.
Last modified: May 8, 2026

